(Translation into most languages at tab to the right)
Mental Health and Addiction
Individuals who struggle with mental health issues and those with any addiction co-exist in almost half of both those populations, as the data shows after decades of research by the National Institutes of Health (NIH). Not surprisingly, individuals who frequently abuse drugs or alcohol are likely to develop a co-occurring behavioral or mental health disorder. There is evidence, for example, that abusers of marijuana have an increased risk of psychosis while those who abuse opioid painkillers are at greater risk for depression. Regular methamphetamine use causes psychosis, anxiety and panic attacks, memory loss and depression. Cocaine users have increased anxiety, paranoia, delusions and depression.
Self-medicating to minimize our inner conflicts is not new, but it has reached new heights in the 21st century – perhaps due to the ease of availability. In Woman of Substances, Jenny Valentish discusses self-medicating at length. She says “In the initial pursuit of partying, people are likely to find themselves drawn to certain families of substances, and they will discover that these additionally offer relief to symptoms of mental illness, distress, or emotional pain.” Why do stimulants calm most people who have ADHD while they have the opposite effect on the rest of us? Why do some antihistamines sedate most people but for some others, cause stimulation? Clearly, their brain chemistry needs something different than the ‘average’ person. It is for the same reason that for many, their drug of choice is a sedative. Their brains need something to turn off the rapid-fire stimulation that can be almost constant.
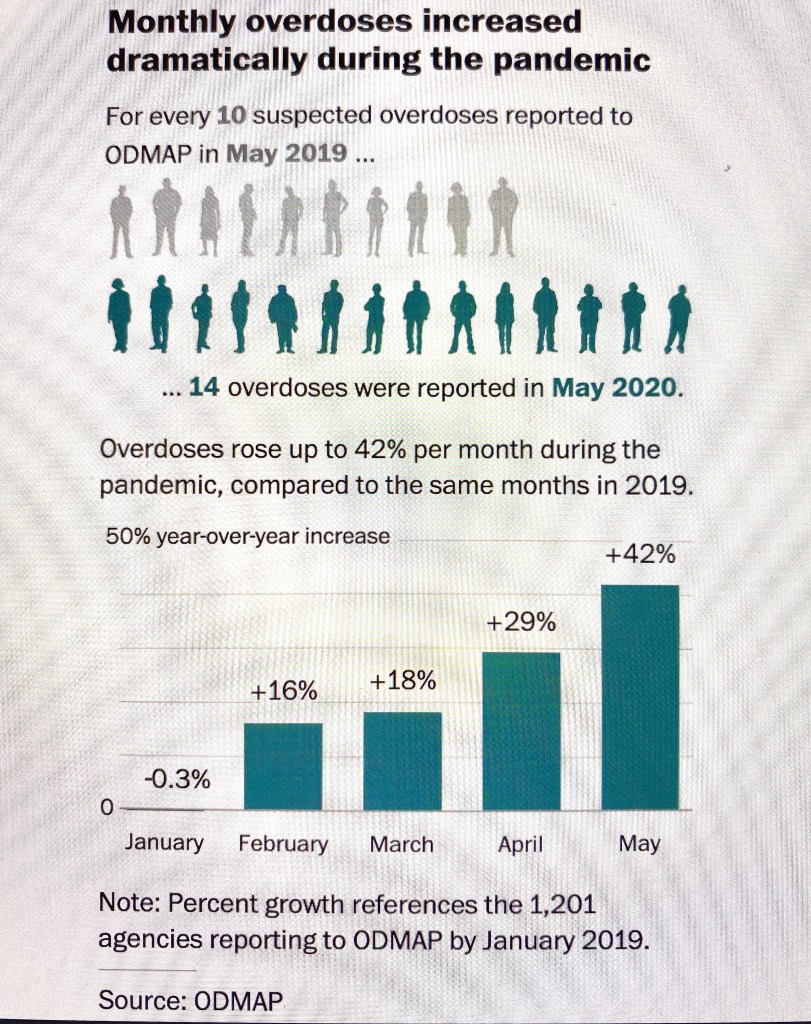
Informative and concerning statistics on mental health in the US:
Continue reading “World Mental Health Day ”